
While the health authorities want to be reassuring, doctors and researchers point out a reality: faced with bacterial meningitis, everything often happens in a few hours. Understanding who is at risk, recognizing the signs and acting quickly can save lives.
An epidemic localized in England, a first signal in France
In Canterbury, in the south-east of England, concern suddenly set in. Fifteen cases of meningitis were recorded in a few days, all serious enough to require hospitalization. Two young people, a 21-year-old man and an 18-year-old high school student, died.
British Health Minister Wes Streeting described a situation “unprecedented”. The investigations quickly revealed a common point: several patients had frequented the Club Chemistry nightclub between March 5 and 7.
A few days later, France was in turn concerned.
A patient returning from England was treated. “The patient was hospitalized and his condition is stable.indicate the health authorities (source: BFMTV). At this stage, no other cases linked to this episode have been identified.
The Health Crisis Center ensures that the situation is monitored “carefully” and that all measures have been taken to limit the risks of transmission.
Behind this vigilance, an essential question arises: who is really exposed when a case is detected?
Who is considered a contact case?
Contrary to some popular belief, meningitis is not easily transmitted in daily life. It requires close, direct contact with the respiratory secretions of an infected person.
According to medical criteria, a contact case is a person who has been exposed to nasopharyngeal secretions (saliva, spit) from a patient in the ten days preceding hospitalization, i.e. the incubation period.
Concretely, this most often involves:
- People living under the same roof;
- Relatives who have had intimate exchanges (kissing, sharing of personal objects);
- Or even very promiscuous groups, like certain communities or prolonged evenings in enclosed places.
This point is crucial: a simple crossing in the street or brief contact is generally not enough to transmit the disease.
In the event of proven exposure, the medical response is rapid and targeted. Preventive antibiotic treatment is offered without delay, sometimes supplemented by vaccination depending on the type of bacteria involved.
But to understand why this reactivity is essential, we must measure the violence of the disease itself.
A rare disease, but symptoms that should never be trivialized
Meningococcal meningitis remains uncommon. However, it is one of the most feared infections in medicine.
The Pasteur Institute recalls that these bacteria are “responsible for the most acute cases”with a mortality rate of around 10%. And even when patients survive, the after-effects can be serious: neurological disorders, amputations, lasting damage.
What makes the disease particularly insidious is the deceptive nature of its beginnings.
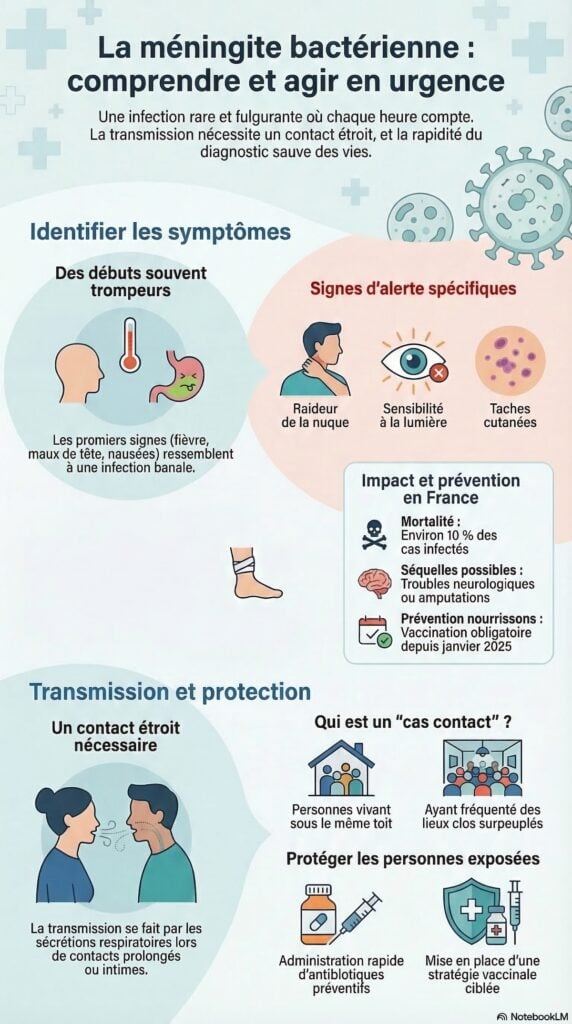
The first signs often resemble a common infection:
- Fever ;
- Headaches;
- Nausea, vomiting.
Then more specific symptoms appear:
- Neck stiffness;
- High sensitivity to light;
- And sometimes spots on the skin (purpura), difficult to spot but characteristic.
The trap is there: these signals can be confused with common illnesses, delaying treatment. In case of doubt, an emergency consultation is necessary and “in all cases, never self-medicate with anti-inflammatories which can mask the symptoms and worsen the disease” specifies Dr. Gérald Kierzek, emergency physician and medical director of True Medical.
However, in the case of bacterial meningitis, every hour counts.
 © NOTeBook LLM
© NOTeBook LLM
Prevent, detect, protect, a race against time
Faced with meningitis, medicine is moving forward with one certainty: speed saves lives.
As soon as a case is identified, everything accelerates. People at risk are contacted, preventive antibiotic treatment is administered to them, and a vaccination strategy can be put in place.
Dr Gérald Kierzek recalls:
“Vaccination is recommended for certain contact cases, in addition to preventive antibiotic treatment. “.
This vaccination depends on the type of meningococcus. For certain serogroups (A, C, W, Y), a specific vaccine is recommended quickly after exposure. For meningococcus B, the cause in several recent cases, the recommendations are more targeted.
At the same time, prevention also involves a broader vaccination policy. Since January 2025, vaccination against meningococci has become compulsory for infants in France, a sign of a desire to better contain this disease.
But beyond medical and public health means, an issue remains deeply individual: recognize the emergency, not minimize the symptoms, and consult without delay.
Today, France has only one case linked to the British epidemic. A situation under control, but closely monitored. Because meningitis reminds us of an essential reality: certain diseases, rare but dazzling, require collective vigilance. Between information, prevention and responsiveness, it is often in the first hours that everything is at stake — where medicine can still reverse the course of things.