For people with
Parkinson’s diseaseoptions run out when tremors, slowness and rigidity resist medication. The reference remains
deep brain stimulationwhich involves major neurosurgery and is only offered to less than 3% of patients. An international team has just tested a form of deep stimulation applied to the scalp, without a scalpel, with a measurable effect on movements.
This technique, called transcranial temporal interference stimulationwas tested in 30 people with early to moderate Parkinson’s in a pilot trial published in eBioMedicine by the Hinda and Arthur Marcus Institute for Aging Research and the Shanghai University of Sport. A single 20-minute session was enough for 70% of participants to have a significant clinical improvement in their motor symptoms, compared to 15% with sham treatment.
How does this non-invasive deep brain stimulation work?
Instead of implanting electrodes in the subthalamic nucleus, the target of deep brain stimulation, researchers place discs on the scalp. Two high-frequency alternating currents, around 2000 and 2130 Hz, pass through the brain. Where they intersect, at the level of the subthalamic nucleus, they create a 130 Hz envelope, close to the parameters used in surgery, capable of modifying the activity of neurons in depth.
For each patient, a brain MRI is used to simulate the current path and adapt the position of the electrodes in order to concentrate an electric field approximately three times stronger in the subthalamic nucleus than in the cortex. The researchers then assessed the MDS-UPDRS-III motor score before and up to 60 minutes after the session. The benefits appeared immediately and were mainly reflected in a reduction in bradykinesia and tremors.
What the Non-Invasive Deep Brain Stimulation Trial Shows
Each participant received a real IT session and a sham session, in random order, without either the patients or the evaluators knowing which one. The beneficial effects of the stimulation were visible immediately after the session and were maintained for at least an hour. The Movement Disorders Society Unified Parkinson Disease Rating Scale (MDS-UPDRS), Part III, which serves as the gold standard for assessing motor symptoms of Parkinson’s disease, showed that “real stimulation” resulted in significantly greater improvements than those observed with placebo at all measurement times.
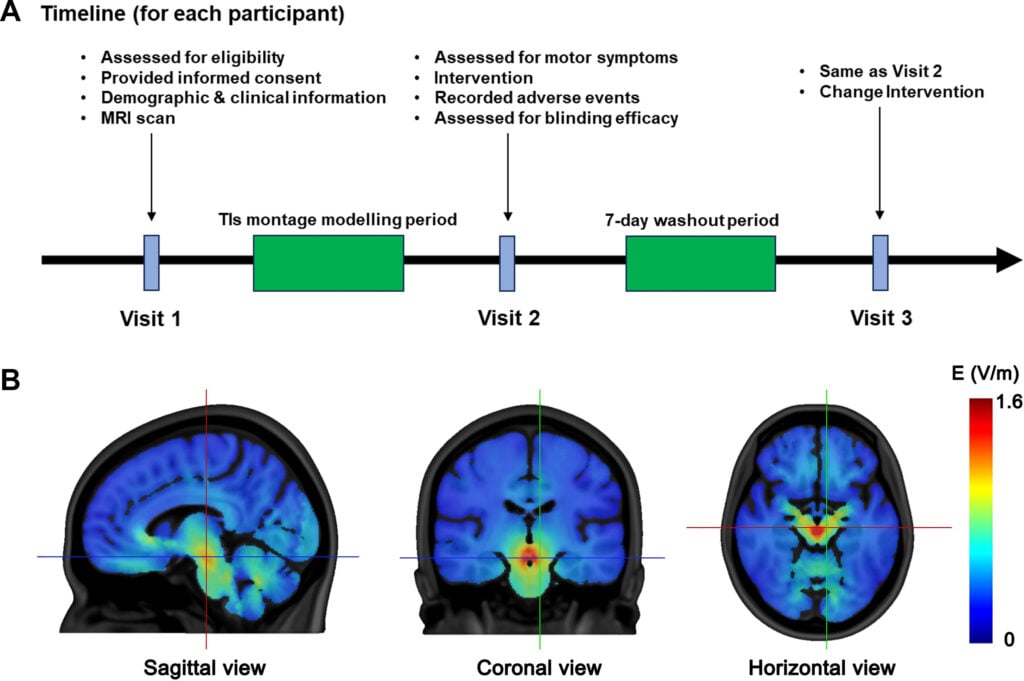 © eBio Medicine
© eBio Medicine
The results highlighted a notable difference: 70% of participants saw a clinically significant improvement after these sessions, compared to only 15% after the placebo. The most significant results were seen in bradykinesia (slowing of movements) and tremors, which are two of the most debilitating symptoms of Parkinson’s disease. On the other hand, progress regarding rigidity and balance has been less regular.
The sessions were well tolerated: no serious complications were reported and the sensations of tingling or heat remained mild, as with the placebo.
“A non-invasive technique like transcranial temporal interference stimulations could one day offer a valuable new option, either before considering surgery or in addition to existing treatments“, said Dr. Brad Manor, principal investigator at the Hinda and Arthur Marcus Institute for Aging Research.
What are the prospects for non-invasive deep brain stimulation in Parkinson’s disease?
Because neurosurgery by deep stimulation only concerns a minority of patients, a technique like
transcranial temporal interference stimulation could, if it confirms its effectiveness, affect many more people, including at earlier stages or too fragile for an operation.
“One of the most promising aspects of this work lies in the possibility of personalize stimulation
depending on the brain anatomy of each patient. This level of precision may become increasingly important as we learn to tailor neuromodulation therapies to different Parkinson’s symptoms and patients.”said Dr. Brad Manor.
For the moment, this is a pilot study: a single short session, without hindsight on the effect of series of stimulations or on cognition or mood. These very encouraging results will therefore need to be confirmed by further studies.