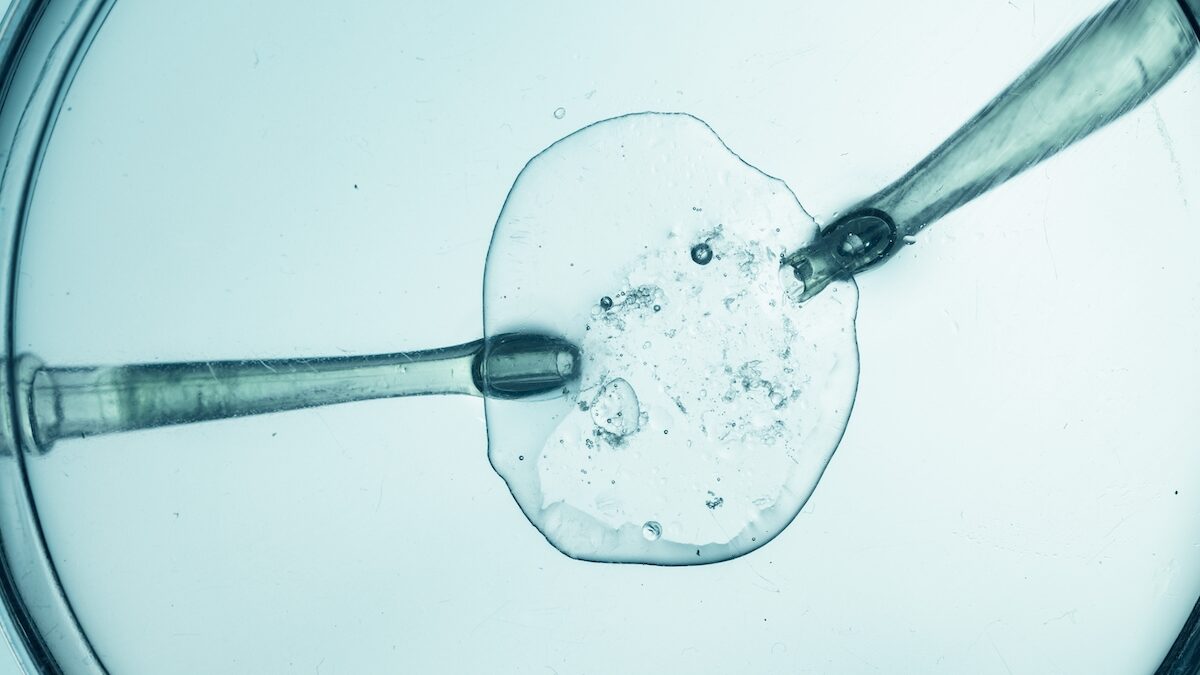
Can we prevent the transmission of incurable genetic diseases while allowing parents to maintain a biological link with their child? This is the challenge that a technique that is still experimental: IVF with three “parents” is trying to meet. Developed in particular in the United Kingdom, it is based on the replacement of a mother’s defective mitochondria with those of a healthy donor. If the first results are encouraging, the researchers call for caution.
A breakthrough to circumvent rare and serious diseases
Mitochondrial diseases, although rare – around 200 new cases per year in France – can cause severe and varied symptoms: neurological disorders, muscular damage, cardiac deficiencies or even diabetes. They are linked to a dysfunction of mitochondria, these “energy plants” of cells.
In almost a quarter of cases, these diseases are due to mutations in mitochondrial DNA, transmitted exclusively by the mother. Until now, women carrying these mutations often had to resort to egg donation, a solution that was sometimes difficult to accept.
Three-parent IVF offers an alternative: retaining the nuclear DNA of both parents while replacing defective mitochondria. As a result, the embryo has three distinct genetic heritages – a first in the field of medically assisted procreation.
A promising but still imperfect technique
The first tests carried out by a British team resulted in the birth of eight children in apparent good health after one year. A notable advance. But researchers remain cautious.
One of the main challenges identified is the phenomenon of “reversion”. During manipulation, it is almost impossible to completely avoid the transfer of mutated mitochondria from the mother to the donor oocyte. However, these defective mitochondria could, in certain cases, multiply more quickly than healthy mitochondria, thus reducing the benefits of the technique.
Long-term unknowns and an open ethical debate
Beyond the technical aspects, biological questions remain. Mitochondria interact closely with the cell nucleus. Introducing a nucleus into a different mitochondrial environment could disrupt these interactions, with consequences that are still poorly understood on cellular metabolism.
Specialists therefore insist on the need for long-term monitoring of children born using this technique, potentially until adulthood. Furthermore, IVF with three “parents” remains prohibited in France, in particular because it involves genetic modification that can be transmitted to future generations.
At the same time, other avenues are being explored, such as the targeted correction of mitochondrial DNA or the destruction of mutations. But according to experts, these approaches are still far from clinical application.
Between a major medical advance and a sensitive ethical area, three-parent IVF illustrates the promises and limits of modern genetic medicine. If it opens a new path for certain families, it also reminds us that every scientific progress requires time, perspective and an in-depth social debate.